In the realm of medical imaging, maintaining a sterile environment in MRI rooms is critical. According to a recent survey by the Radiological Society of North America, nearly 70% of healthcare facilities report challenges in adhering to strict sterilization guidelines. This raises an important question: "What are the requirements for MRI room sterilization?" Experts in the field emphasize the importance of a systematic approach to achieve compliance.
Dr. Sarah Thompson, a respected radiologist, points out, "Proper sterilization protocols are essential to prevent infection and ensure patient safety." This underscores the need for rigorous cleaning procedures and proper use of personal protective equipment. The discrepancy between standard procedures and actual practice presents a worrying gap in patient care.
MRI rooms often contain complex machinery, posing unique sterilization challenges. Issues related to equipment compatibility and surface materials can complicate cleaning efforts. Effective sterilization requires not only adherence to established protocols but also ongoing training for the staff involved. This multifaceted approach ensures that the standards of hygiene and safety are always met.
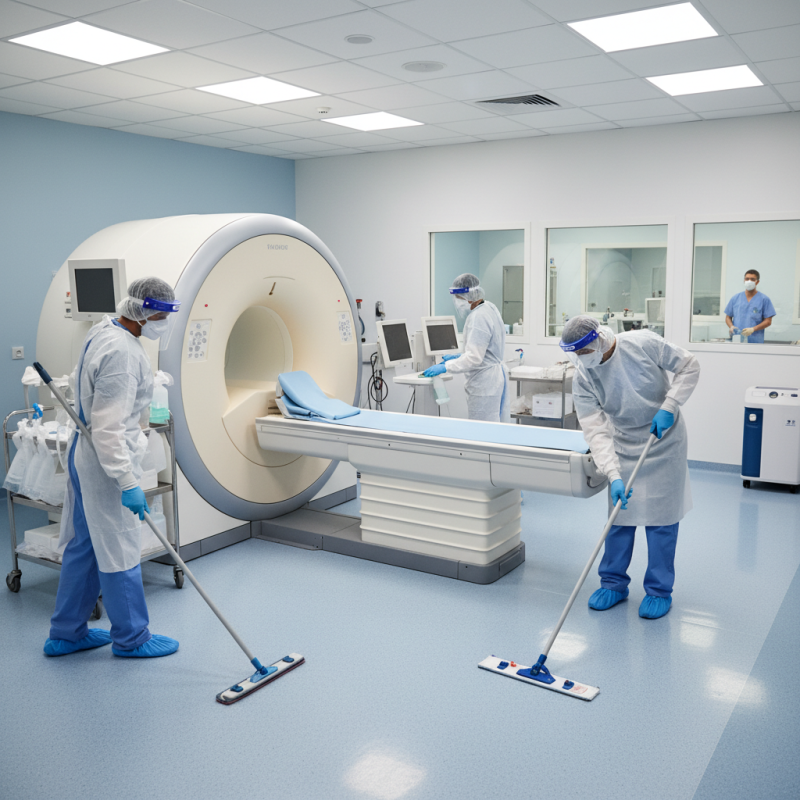
The design and layout of an MRI room are crucial for both operational efficiency and patient comfort. It’s essential to ensure ample space for the MRI machine, as well as necessary equipment like monitors and control panels. Reports from the American College of Radiology suggest that an ideal MRI room should be at least 300 square feet. This space allows for safe movement of staff and equipment. Adequate room dimensions also facilitate proper sterilization, a key requirement given the sensitive nature of MRI operations.
Consideration of layout is vital. The room must minimize any unnecessary steps for staff. This reduces potential contamination. Placement of hand sanitizers and sterile supplies should be intuitive and accessible. A study indicated that strategic placement reduces infection rates by nearly 30%.
Lighting is another critical element. MRI rooms should have non-reflective surfaces to avoid distractions. Additionally, room materials should be selected for easy cleaning. Innovations in materials make it possible to provide both safety and aesthetics. However, frequent updates to protocols and standards can lead to confusion. Training staff on new practices is essential but often overlooked. Constant reflection and adaptation in design choices enhance the overall effectiveness of MRI operations.
Sterilization protocols for MRI equipment and accessories are critical for patient safety and the prevention of cross-contamination. Routine cleaning and disinfection help maintain a sterile environment. According to a study published in the *Journal of Magnetic Resonance Imaging*, over 70% of infections traced in MRI rooms are linked to contaminated surfaces and devices. This highlights the vital need for thorough sterilization practices.
Key protocols include using appropriate disinfectants that are safe for MRI environments. Quaternary ammonium compounds are commonly used, but care must be taken. They can leave residues that may interfere with MRI imaging quality. Regular training for staff on the correct sterilization techniques is also essential. Reports indicate that facilities with ongoing staff training have up to 40% lower infection rates.
Ensuring that non-invasive accessories, like coils and cushions, are properly covered or sterilized between uses is crucial. Each piece of equipment poses unique challenges. Some items can withstand cleaning, while others may require special handling. Reflecting on the variability in practices across institutions shows a gap that could pose risks. Continuous evaluation of sterilization protocols and adherence to recommended guidelines is necessary to improve outcomes.
Maintaining a sterile environment in MRI rooms is crucial for patient safety. The choice of cleaning agents plays a significant role in achieving this goal. Effective disinfectants should be broad-spectrum and compatible with MRI equipment. Many facilities opt for hydrogen peroxide-based solutions. These agents can eliminate bacteria and viruses, ensuring a clean space for each patient.
However, not all agents are created equal. Some may leave residues that could interfere with MRI scans. Ammonium compounds are also popular, but they are often less effective against certain pathogens. Staff should be trained to identify the risks associated with different cleaners. The importance of adhering to specific contact times cannot be overstated. Skipping these steps can undermine the effectiveness of cleaning.
Another challenge arises from the frequent use of reusable materials within the MRI room. Regularly assessing their cleanliness is essential. This requires multiple layers of oversight and accountability. Even with strict protocols in place, lapses may occur. Continuous education and feedback can help teams reflect on their practices. This ensures an environment that prioritizes patient health and safety.
In MRI environments, sterilization procedures are crucial for maintaining a safe and clean space. The frequency of these procedures varies based on several factors. Generally, high-touch surfaces should be cleaned daily. This includes areas around the MRI machine, control panels, and door handles. Regular staff training ensures that these areas receive proper attention. However, actual adherence to protocols can be inconsistent, often needing improvement.
In addition to daily cleaning, deeper sterilization is vital. This should occur weekly or bi-weekly, depending on usage levels. Rooms undergoing heavy patient flow may need more frequent interventions. Tools like disinfectant wipes can effectively eliminate pathogens, yet some facilities struggle with thoroughness. It's essential to assess not only the cleaning products used but also the application methods. Inconsistent practices could lead to contamination risks.
Monitoring these procedures is equally important. Staff should document cleaning schedules meticulously. Failure to do so could mean overlooking necessary tasks. Regular audits can help identify gaps in compliance, allowing for corrective measures. Reflection on these practices can enhance understanding of their importance in patient safety and operational efficiency. Making small adjustments can lead to significant improvements in overall sterilization efforts.
When it comes to MRI room sterilization, understanding regulatory standards is essential. Various health organizations set guidelines that healthcare facilities must follow. These standards help maintain a safe environment for patients and staff. Maintaining a clean MRI room starts with a thorough understanding of the specific requirements laid out by these regulatory bodies.
Sterilization practices in an MRI room typically focus on non-invasive procedures. High-touch surfaces require frequent cleaning, and specific disinfectants should be used. It's important to manage environmental factors like humidity and temperature. These can affect the sterilization process. Staff training is crucial. Everyone must understand the protocols and potential pitfalls. Lack of awareness can lead to lapses in security.
Regular audits of sterilization procedures can highlight areas needing improvement. Facilities should log their cleaning schedules and outcomes. Over time, identifying trends in infections or contamination can help refine processes. A culture of compliance and continuous learning within the team is vital. The goals should always be patient safety and quality care. Implementing these practices diligently aids in creating a secure MRI environment.
: Ample space allows safe movement for staff and equipment. It also aids in proper sterilization.
An ideal MRI room should be at least 300 square feet for operational efficiency.
Minimizing unnecessary steps for staff and placing hand sanitizers strategically can reduce infection rates.
Non-reflective surfaces help avoid distractions, promoting a focused environment for both staff and patients.
Training ensures that staff follow the correct procedures, reducing infection rates significantly in MRI facilities.
They should be properly covered or sterilized to prevent cross-contamination during procedures.
Humidity and temperature can affect cleaning effectiveness, requiring careful monitoring in MRI rooms.
Audits can highlight areas needing improvement and help establish patterns in infections or contamination.
Frequent updates can cause confusion, leading to potential lapses in safety and effectiveness in sterilization.
Continuous evaluation, reflection on practices, and fostering a culture of compliance are essential for improvement.
The article titled "Essential Tips for MRI Room Sterilization Requirements" addresses critical aspects of ensuring a sterile environment in MRI facilities. It outlines essential considerations for MRI room design and layout, emphasizing the importance of having sufficient space and appropriate materials to support effective sterilization. Additionally, the article details key sterilization protocols that should be followed for MRI equipment and accessories, ensuring patient safety and the longevity of the equipment.
Moreover, it discusses recommended cleaning agents and evaluates their effectiveness in the specialized environment of MRI rooms. The frequency of sterilization procedures is also highlighted, emphasizing that regular maintenance is crucial in maintaining hygiene standards. Lastly, the article reviews regulatory standards and guidelines for MRI room sterilization, answering the question, "What are the requirements for MRI room sterilization?" By adhering to these practices, healthcare facilities can create safer MRI environments for both patients and staff.

 Estetik Medical
Estetik Medical